Ep 6 – Hepatic Clearance For The FRCA Primary
8 November 2024
Contents
This episode explores Hepatic Clearance of drugs and moves on to First and Zero Order Kinetics, these concepts are the building blocks for exponential decay that occurs in pharmacokinetic systems, check out Michaelis-menten enzyme kinetics and the multi compartmental madness / sevoflurane jaunt episodes for more.
Clearance is a pharmacological concept used to consider the rate or removal of a drug from a system
It is important to appreciate that clearance of a drug does not necessarily correlate with its offset, as drug action is dependent on enough drug saturating enough receptors or intracellular enzymes.
What is Hepatic Clearance?
Hepatic clearance refers to the liver’s ability to remove drugs from the bloodstream. It involves metabolism and biliary excretion, influencing the drug’s half-life and overall elimination.
Contextualising Hepatic Clearance
- If a drug chiefly operates from within the intravascular space then its pharmacological offset may correlate more with clearance
- If it chiefly works from within a cell then it’s less likely to correlate.
- Clearance is defined as: the volume of blood (say 10 mls) cleared entirely of drug per unit time Mls/minute
- Sometimes indexed to body mass. (mls/kg/min)
- Drug elimination is ‘different’ i.e. the irreversible removal of drug from the body.
- Drug clearance is the volume of blood cleared of drug.
Yet again we have a number that ends up being almost entirely theoretical if taken on its own as verbatim. Just because the body could clear a litre of blood of a drug in a given time frame, doesn’t mean that there is that amount of drug available to hoover up. If ther agent has a high volume of distribution then it is off lurking elsewhere and by its very suggestion of a high VOD, not much is in the plasma!
Deranged Physiology describes diltiazem and felodipine – both similarly high clearances 600-800ml/min but as felodipine has a high VOD its elimination half life is prolonged.
It is important to remember that singular physiological/physical concepts often struggle to completely hold up in the face of reality. I think of this as – we’ve tried to organise and account for systems and describe them formulaically , however, deep down there are confounders that knock things out by a few decimal points, but on the face of it these formulas mostly work.
Define or Die
Clearance is defined as: the volume of blood (say 10 mls) cleared entirely of drug per unit time Mls/minute
This is the fundamental overall clearance a system achieves, however!
There are multiple sub systems mopping up bits of drugs and their varyingly soluble metabolites!
So we will end up having to think about:
- Renal clearance
- Hepatic Clearance (metabolism or just into bile)
- Pulmonary Clearance
Don’t conflate first-pass metabolism and hepatic clearance — the former involves portal blood flow only.
Hepatic Extraction Ratio and Intrinsic Clearance
Digging into hepatic clearance there are a few more important concepts - Hepatic Extraction Ratio (HER)
- Extraction ratio: the amount of molecule removed from blood from entry to exit of an organ,
- Extraction ratio = 1- Concentration of molecule going out (venous) / Concentration of molecule going in (arterial)
This concept also could be applied to oxygen extraction by organs (Ficks Principle)
There are a few factors which influence the extraction ratio, the chief one is the amount of drug that is unbound (as a fraction)
Intrinsic clearance (hepatic) The ability of the liver to metabolise drug if it was freely thrown as much drug as it could possibly desire (i.e. devoid of constraining factors like blood flow, protein binding, solubility)
As blood flow across the liver goes up : Extraction ratio will decrease
These can be sub classified dependent on the intrinsic clearance of the agent
- Low intrinsic clearance = greater drop in HER - Hepatic clearance of the drug will not increase much with blood flow
- High intrinsic clearance = HER increases in a fairly linear manner
To summarise this, if the intrinsic clearance is really high and the liver hoovers up a drug like no tomorrow – then its clearance is often constrained by blood flow to the liver, Whereas if the Liver cant be bothered to clear something then you can present as much as you like to it and it simply won’t get around to it, a feckless waiter not taking your order!
Drugs which have a high clearance like propofol exhibit cardiac output dependent clearance
This will make more sense if you think about it in the concept of Michaelis-Menten kinetics / Laws of mass action – we will do this in another podcast
Pulling back up to the surface
Hepatic clearance is influenced by the efficiency of the liver in removing the drug and the blood flow to the liver.
There is a formulaic representation of this.
QH = hepatic blood flow
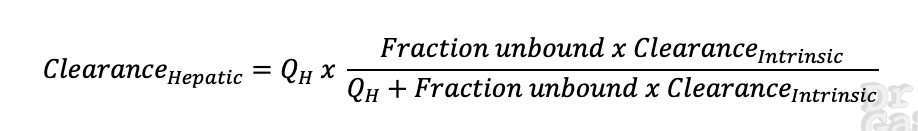
How to apply hepatic clearance clinically?
Lots of concepts there, but limping ourselves back to Hepatic extraction ratio reality.
- Drugs with High HER = Propofol -Morphine – Ketamine
- Drugs with Low HER = Rocuronium – Lorazepam – Diazepam – Theophylline
So in low flow states things like propofol can build up more as more often than not the liver would be hoovering it up. The kidneys also metabolise a small fraction of propofol; anhepatic propofol clearance has been demonstrated during the hepatectomy phase of liver transplantation.
Whereas rocuronium, wont be terribly altered if your patients BP was 70 for the entire case because the hepatocytes are inherently feckless, as the rocuronium trundles past them (comparatively).
So by extension we are probably quite interested in what states alter hepatic blood flow.
Hypovolaemic shock states naturally lead to diminished flow
Early bounding flushed septic patients have increased flow, once they get cold and shut down they have less.
ITU drugs – vasoconstrictors generally reduce flow – inodilators increase C.I. >increase hepatic blood flow.
Summary
Get the idea of high intrinsic clearance (i.e very metabolically / enzymatically active) into your mind and remember that if youre delivering lots of drug to a nice busy/keen hepatocyte you’ll clear lots of drug.
As having this grasp means when you approach first/zero order enzyme kinetics your brain will already be there!
Clearance = eradication of drug from a volume of blood
Elimination is eradication of drug from entire system irreversibly
Renal blood flow will also influence drug clearance, but the concept of extraction ratios didn’t seem to come up as much…
Enterohepatic Recycling
Enterohepatic recycling – Drugs > Bile > that are glucuronide conjugated may be hydrolyzed in the gut thanks to bacteria secreting gluconoridase….> If this happens to be a lipid soluble drug it can re reabsorbed into portal flow. Alterations in gut microbiome can lead to changes in plasma drug concentration (possibly why ABX mess with the COCP)
Read me Next: Michaelis Menten Enzyme Kinetics
References
Thanks for listening. Take it day by day, don't overcook yourself — keep studying.
Transcript
18 min listenRead the full transcript
Introduction and Podcast Overview
00:00-00:34
Please listen carefully. Hello, and welcome to Gas, Gas, Gas, your one-stop podcast for the FRCA primary exam. This podcast will fill your brain with information. Listen to it, think about it, and check out the show notes on the website. There, you will find the core diagrams you need to be able to draw and describe for the exam.
This podcast can squeeze into your day. Listen while you’re driving to work, cooking dinner, maybe when you’re on call, or in the gym. Eventually, the revision is going to end, but for now, expect facts, concepts, model answers, and the odd tangent. Remember to rate and follow the show to hear much, much, much more.
Defining Drug Clearance
00:35-01:32
Hi everyone, this is James at Gas Gas Gas. Today we are looking at drug clearance. Clearance is all to do with how the body gets rid of stuff. This stuff includes drugs, but also you could think it could include creatinine, toxins, ammonia, urea, all these bits and pieces that the kidney clears, the bilious products of your haemoglobin tidying up mechanisms and bile and biliverdin and all those sorts of things.
That’s all clearance of stuff from within the body to a route which it can be eliminated out of. You could also think about how when you breathe out sevoflurane after an anaesthetic when you’ve cleared their circuit, that’s clearance in some way, shape, or form as well.
Just to confuse, clearance is often described in mils per minute, and this is how many mils of blood can be entirely cleared of an agent in one minute, which is a bit of a weird unit in my eyes, but it seems to work.
Clearance vs Offset Time
01:32-02:43
However, there are some caveats with clearance, as there are with almost everything to do with the human body - it’s important to appreciate that clearance of a drug does not necessarily correlate with its offset time. Remembering that the action of a drug is dependent on the concentration of that drug at its receptor or its intracellular enzyme.
You can think about this a bit further. So if a drug chiefly operates from within the intravascular space, then its offset might correlate a bit more with its clearance. If, however, the drug you’ve given chiefly works from within a cell, then it’s going to be less so.
Volume of Distribution and Propofol Example
02:43-03:31
You could extend this further to thinking about the drug and its volume of distribution, because you can imagine that a drug that’s got really high volume of distribution means that most of that drug’s off floating around in adipose tissue and inside cells, nowhere near the intravascular space. And therefore, even if theoretically the clearance was absolutely mega, there’s just no drug in the intravascular space to clear. So it doesn’t really bear relevance to its onset offset time.
A good example of this is propofol. So you give a dose of propofol, the plasma concentration is really high. Your blood flow to your brain, your heart, and some other key organs is really quite high. So, loads of that propofol goes to the brain. But then, if you don’t give any more, lots of that propofol redistributes, evens out, it soaks into the fatty tissues, the muscular tissues and the concentration in the brain goes down.
The total amount of propofol in the human has not changed, but where it is has, and therefore it’s offset, but the propofol’s still in them. It’s just not in the right place to work.
Clearance Units and Limitations
03:31-04:47
Sometimes this unit of mils per minute can get indexed to body mass, i.e. mils per kilo per minute, which is perhaps something that makes a little bit more sense than the initial unit that doesn’t take into account the size of the person.
I suppose what I’m trying to say when referring to the volume of distribution of a drug and the onset offset times of propofol relative to the clearance of propofol is that taken on its own, clearance is another not very useful marker of pharmacokinetic activity that on its own verbatim doesn’t resemble much of a useful metric for actually working out what a drug does to a person.
However, it becomes relevant when considering particular drugs in particular disease states, whereby you think actually accumulation is the issue, or they’re clearing the agent so rapidly because they’re on renal replacement therapy, they’d actually need to give them more, although that rarely is the case.
So, the concept that often applies to many things in medicine is important to remember that singular physiological or physical concepts often struggle to hold up completely in the face of reality. This is probably because as humans we have tried to organise and account for systems and describe them in a formulaic manner. However, deep down, there are confounders that knock things out by a few decimal points. However, on the face of it, these concepts work and they’re useful when applying it to a patient in a simple manner.
Types of Clearance
04:47-05:34
So as I alluded to, clearance as a singular concept isn’t terribly useful and it actually breaks down into multiple different subtopics, i.e., hepatic clearance, renal clearance, pulmonary clearance, and also you could be thinking about the intercompartmental clearances that are very useful in the pharmacokinetic models used to describe a number of drugs, propofol and remifentanil being the chief ones, but there are models for ketamine and alfentanil too.
I’m going to focus on this podcast on hepatic clearance because there’s a few concepts that will ultimately illustrate some other physical and chemical things you’ve got to learn about. And it really quite confused me when I first looked at it, so it’s good learning for everyone.
First Pass Metabolism vs Hepatic Clearance
05:34-05:52
First things, don’t conflate first pass metabolism and hepatic clearance, chiefly because first pass metabolism is entirely dependent on portal flow only, and not portal plus hepatic arterial flow.
Key Concepts: Extraction Ratio and Intrinsic Clearance
05:52-06:43
There are a few other important concepts when thinking about hepatic clearance. There’s a term called the extraction ratio, and this is the amount of molecule removed from the blood from entry into the liver to exit from the liver. This concept is applied elsewhere and is a means of calculating oxygen consumption and, for example, cardiac output in some situations by measuring the concentration going in and the concentration going out, if you know the uptake. That’s another concept entirely.
There’s another new term to learn: intrinsic clearance and this is particular to the liver in this case, but might be particular to other organs too, i.e., intrinsic clearance being the ability of the liver to metabolise drug if it was freely thrown as much drug as it could possibly desire, i.e. devoid of constraining factors like solubility, blood flow, protein binding, etcetera.
Railway Station Analogy for Intrinsic Clearance
06:43-08:03
I like to try and think about things in slightly left of field manners in order to get a concept organised in my noodle. So when I think about intrinsic clearance, I’m imagining the world’s most efficient railway station, and you can throw thousands and thousands and thousands of humans at it, and it just keeps mopping them up until that railway station finally bottlenecks and says that’s ten thousand humans in a minute, that’ll be the intrinsic clearance of the railway station.
If you start chucking more humans at it, it’ll jam up and won’t process them. But if you chuck only a thousand humans at it, it’ll still clear them through. So there’s an availability element to think about here, and a how much can get through the pipes element to think about.
The contrary to that situation might be you’re throwing ten thousand passengers past this railway station every hour, but actually loads of people don’t bother getting off because they know they’re just gonna get stuck in traffic. And the train station, the railway station, just can’t be arsed to clear the people. So you just get stuck there queuing for hours trying to get off. So the people don’t bother. They just keep staying on the rail line and getting off at the next stop instead.
And this would be an example of low intrinsic clearance, i.e., the liver just can’t be arsed. It only takes up like two percent of the passengers and the rest just have to float on past, come round again, hopefully get off.
The final step of this analogy is how fast the trains are going past the station. If that train’s rambling along and moseying along, then the railway station might be able to take some more people off. Whereas if that train has piled through the train station in a minute it’s gone, then fewer people are going to be able to get off.
Blood Flow, Extraction Ratio, and Intrinsic Clearance Relationships
08:03-09:45
Pulling these three concepts back together of blood flow across the organ, the ability of the organ to clear the drug, and then the ability of the organ to extract the drug from the blood, we can then start thinking about how this applies in reality. These all interplay to influence how good a drug is cleared or how badly a drug is cleared in either high or low flow states, i.e., think of your bounding septic person versus your cold, sepsis, shutdown, really knackered dying person.
The rule of thumb is as blood flow across the liver goes up, the extraction ratio decreases because it’s just zooming past. But then if you take into account the intrinsic clearance in this situation. If there is a low intrinsic clearance, then there will be a greater drop in hepatic extraction rate. I.e., hepatic clearance of said drug will not really increase much with blood flow because it can’t be arsed. It’ll deal with 10 a minute, and if you give it 100 per minute, it’s still just going to deal with 10 a minute.
Whereas something with high intrinsic clearance, the hepatic extraction ratio increases in a fairly linear manner with the blood flow, because if it’s some super duper organised hepatocyte, and it’s like, “yeah, give me all the drugs.” And the body’s like, “yeah, here’s all the drugs.” And it’s like, “I’m going to keep going. Give me more drugs, more drugs,” and it just keeps going and going and going until it reaches its limit, and then it will flatten out.
High vs Low Intrinsic Clearance
09:45-10:45
To put that into clearer terms, if the intrinsic clearance, i.e., the drive of the hepatocyte, is really high and the liver can hoover up that drug like no tomorrow, then its clearance is often constrained by the blood flow to the liver. The counter being, if the liver just can’t be bothered, you can present as much as you like, and it just won’t do much. It’ll always clear one unit, then it’s quite a fixed clearance rate.
An excellent example of that is alcohol, hence why one unit takes an hour to clear, and if you drink thirty units, it takes thirty hours to clear, because the liver can only do a unit per hour. So that has a low intrinsic clearance because that system gets rapidly saturated.
You might have noticed when you’re really, really hungover that you feel awful, awful, awful, awful, awful, awful, and then suddenly you feel rapidly very better. And that’s likely this at play and the metabolic byproducts of the alcohol metabolism that makes you poorly. Also, probably have a low intrinsic clearance, hence why it takes a while and then it suddenly is done.
Connection to Michaelis-Menten Kinetics
10:45-11:02
This concept plays out on a formulaic and graphy type level with Michaelis-Menten kinetics, and that’s for another podcast. Talking about enzyme saturation, the Vmax, i.e. the intrinsic clearance of that system, etcetera. We’ll do it in another podcast.
Clinical Examples: High vs Low Hepatic Extraction
11:02-11:44
So we’re going to scrape ourselves back towards reality to tell you that there are some drugs with a high hepatic extraction rate: propofol, morphine, ketamine, whereas there are some drugs with a low hepatic extraction rate: rocuronium, lorazepam, diazepam, and theophylline.
How does this apply? In a low-flowing state, things like propofol are more likely to build up, as the liver is really not getting the drug with which to clear, so it accumulates. Whereas rocuronium, its clearance rate won’t be terribly altered because the clearance of rocuronium with its low hepatic extraction ratio is already pretty fixed unless you’re really just getting no blood flow to your liver whatsoever. But then if people are that sick and they’ve been anaesthetised, we probably aren’t going to wake them up.
Factors Affecting Hepatic Blood Flow
11:44-13:15
So by extension, arguably in an exam, and maybe in real life even, we might be interested in states that alter hepatic blood flow. And I’m sure we can think of some. A hypovolaemic person is going to have a low flow state in their liver.
Interestingly, sepsis can do both if you’ve got that bounding, florid, vasodilatory, high cardiac output septic phase - hot, sweaty, flushed person, they actually have a higher hepatic blood flow, although it’s seemingly quite wasted because they’re just hosing blood all around their body. However, once they get cold and they tip into that vasoconstricted periphery shutdown, really sicky poorly septic state, then their hepatic blood flow goes down.
Also, although we’re probably getting into the depths of minutiae that don’t really play out in clinical practice very much in terms of relevance is that there are some drugs that also are going to influence hepatic blood flow. So, vasoconstrictors all generally reduce blood flow to your liver - we’re talking your noradrenaline, your metaraminol, etcetera. Whereas your inodilators - we’re thinking here your dobutamine, your adrenaline infusion, your milrinone, levosimendan, if you’ve got the luxury of having that drug, would increase your cardiac index, increasing your hepatic blood flow.
How these would actually bear out in terms of altering your apparent clinical state, it’s probably pretty minimal stuff.
Zero-Order vs First-Order Kinetics
13:15-14:18
I have introduced a bunch of new terms when discussing hepatic clearance. Just to bamboozle you more, one last thing, because it’ll tie in nicely with when we do Michaelis-Menten kinetics. We remember that state whereby the liver only clears ten molecules per minute, can’t be arsed any more. Even if you throw as much blood flow at it, it’s just doing 10 per minute. This is a situation of zero-order kinetics, i.e. it’s a flat rate of clearance that is not influenced by flow.
Whereas our dear, very hard working hepatocyte, chomping through drug as best it can and it’s just got loads of capacity to do it, it takes a while to saturate that enzyme. And that curve of flow to enzyme activity that’s working in that little hepatocyte, that nice curve that you can imagine exists, would be first-order kinetics.
Most drugs exhibit first-order kinetics unless you really, really, really, really, really saturate the human and bind up all those enzymes. Only some drugs exhibit zero-order kinetics: alcohol and phenytoin are the ones that jumped to my mind.
Clearance vs Elimination
14:18-14:36
So to remember, clearance equals eradication of drug from a certain volume of blood, not to be conflated with elimination, which is the eradication of a drug from an entire system irreversibly, i.e., it’s out and never coming back.
Enterohepatic Recycling
14:36-15:36
I’m just gonna add this at the end. So there’s a little concept that comes up in regards to liver clearance of drugs that talks about something called enterohepatic recycling, i.e., drugs that are cleared into the bile, but then delightfully thoughtful GI bacteria find these neatly conjugated glucuronides, and they go, “Oh, you know what, I can hydrolyse that in the gut because I secrete glucuronidase.”
Now you can imagine if this happens to a lipid soluble drug, it now can be reabsorbed across your GI membrane, back through your liver, back off to the rest of the body, and it can be recycled - enterohepatic recycling. This is a useful thing to talk about. It possibly happens with a few opiates, but also is a suggestion as to why alterations in your gut microbiome when you’re given antibiotics, can sometimes alter the plasma concentration of your combined oral contraceptive pill because of the way the GI bacteria handle the oestrogens. Fun times.
Conclusion
15:36-16:13
Anyway, thank you very much for listening. This is Doctor James on Gas, Gas, Gas. Next time, well, I think it might be volatile anaesthetics. See you then.
If you found it useful or awful, please like and subscribe and rate the show. Definitely check out the show notes for those diagrams and the detail of this content. It is a bucket of content to get to grips with. Keep working at it and you will get better, faster and stronger. It is vital to keep your interest alive for the science that we’re covering and not overcook yourself. You will be amazed by what you know come exam day. Don’t freak out, keep studying.
Enjoyed this? Review on Apple Podcasts Rate on Spotify
Support the show Help keep the lights on SBA question bank @ Teach Me Anaesthetics
